Why antibody tests won't help you much
Many tests are inaccurate, some look for the wrong antibodies and even the right antibodies fade away, said experts


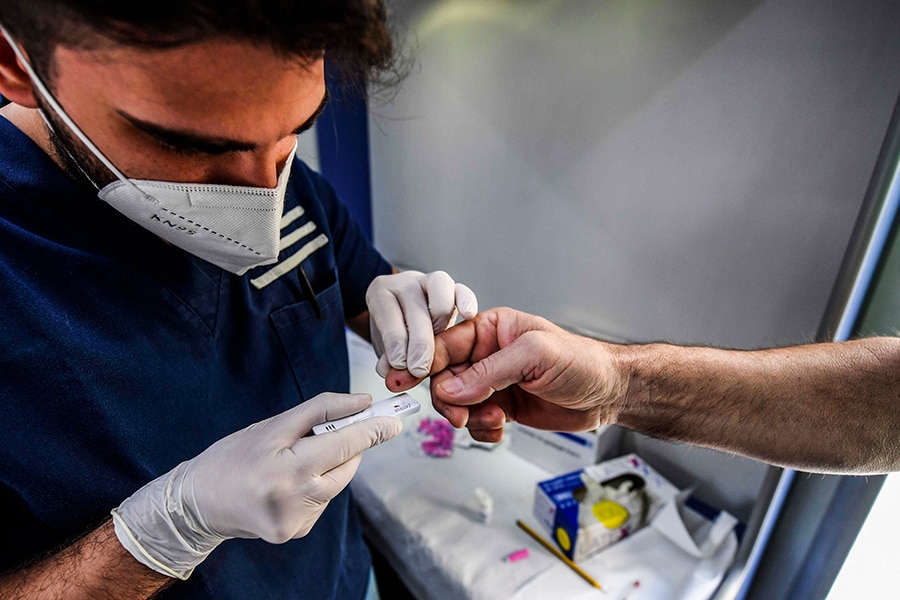 Naples, Campiania, Italy, 2020/06/15: A medical worker handles an antibody rapid serological test for COVID-19 following a finger prick blood sample from a man.
Naples, Campiania, Italy, 2020/06/15: A medical worker handles an antibody rapid serological test for COVID-19 following a finger prick blood sample from a man.
Image: Salvatore Laporta/KONTROLAB/LightRocket via Getty Images)
Getting an antibody test to see if you had COVID-19 months ago is pointless, according to guidelines issued this week by a major medical society.
Many tests are inaccurate, some look for the wrong antibodies and even the right antibodies fade away, said experts at the Infectious Diseases Society of America, which issued the new guidelines.
Because current tests cannot determine if someone is immune, the society said, they “cannot inform decisions to discontinue physical distancing or lessen the use of personal protective equipment.”
Antibody testing generally should be used only for population surveys, not for diagnosing illness in individuals, the panel said. But its guidelines described two situations in which antibody testing could be used when the normal diagnostic tests for the virus — called PCR tests — failed or were likely to fail.
People who felt sick weeks or months ago and now wonder if they are immune to COVID-19 “probably shouldn’t bother” getting an antibody test, said Dr. Angela M. Caliendo, a testing expert at Brown University’s Alpert Medical School and a member of the society’s expert panel.
Many New Yorkers fell ill in the spring, could not get tested then and now wonder whether they had the disease and are immune the panel concluded that current antibody tests cannot answer that question.
“We don’t really know if a positive test means you’re protected,” Caliendo said. “If you were sick back in March, you probably don’t have antibodies any more and if you were only mildly sick, you may not have gotten antibodies.”
Moreover, she said, “if you live in a low-prevalence area, you have a much higher likelihood of getting a false-positive test, meaning you may think you are protected but you aren’t.”
Despite the flaws of antibody tests, recent studies of patients who definitely were infected suggest that they have long-lasting immunity and that it is very unlikely they will get reinfected.
That may be because white blood cells known as B and T cells, which are “primed” to recognize and attack the coronavirus, remain in circulation long after antibodies have faded away. But B and T cells are not analyzed by common antibody tests.
Other experts echoed the society’s recommendation against individual antibody tests.
Michael T. Osterholm, director of the University of Minnesota’s Center for Infectious Disease Research and Policy, called diagnostic clinics that charge individuals for antibody tests “snake oil salesmen.”
Antibody tests — which analyze blood for proteins produced by the immune system that bind to the outside of the virus and neutralize it — are useful mostly for surveys of large populations to see roughly how many people have had the disease, the society said.
Even for that purpose, only tests that are correctly positive more than 96% of time and correctly negative at least 99.5% of the time should be used, according to the guidelines.
Very few of the dozens of tests made in this country, Europe and Asia that the panel looked at met those standards, Caliendo said. None can be done at home or immediately in doctors’ offices, and the best are assays known as Elisa or CIA (chemiluminescence immunoassay). Tests using paper strips were less consistently accurate, the panel found.
With two exceptions, antibody tests should not be used to diagnose individual infections, the society said. When a patient has all of the symptoms of COVID-19, including X-ray evidence of pneumonia, but still comes up negative on repeated diagnostic PCR tests for the virus, an antibody test may be useful.
Ideally, it should be given not immediately after symptoms appear, but three to four weeks later — “the sweet spot,” Caliendo said.
(PCR nasal swab tests may come up negative after the virus migrates from the nose and throat to the lungs, Caliendo explained but the body may not produce enough antibodies to be detectable in the blood until more than two weeks have passed.)
The tests can also be used for diagnosis when a doctor suspects a child has multisystem inflammatory syndrome, a rare but serious complication of COVID-19 in children. Because it is not known how long after the initial infection this inflammation begins, doctors should do both a PCR test and an antibody test, the guidelines said.
The Centers for Disease Control and Prevention also issued guidelines for using antibody tests they were last updated Aug. 1. The guidance is based on validations of test kits by the National Cancer Institute, while the infectious disease society reviewed test results from all over the world, said Dr. Kimberly E. Hanson, a testing expert at the University of Utah Hospital who was also on the expert panel.
The panel found it hard to decide which tests were worth recommending.
The Food and Drug Administration’s decision in April to approve tests without even reviewing their safety and efficacy data “turned out to be a problem,” Hanson said. “The market was flooded with poorly performing tests.”
After harsh criticism from testing experts and Congress, the FDA reversed that decision in May and gave test-makers 10 days to prove their tests were accurate or be banned from selling them.
On Wednesday, the Department of Health and Human Services, citing an executive order from President Donald Trump, said that laboratories that developed their own in-house tests for the virus did not have to pass FDA review. The order does not apply to the commercial tests the panel analyzed.
The tests still on the market now are better but still not good enough, experts said.
The panel examined 9,500 papers describing test validation and found only 47 worth considering. “It was a mishmash of stuff,” Hanson said.
Caliendo said, “We naively thought this would be simple. There are not a lot of high-quality results on these tests.”
Even in those 47 papers, the same tests did better or worse in different studies, they said.
Tests that do not detect so-called IgG antibodies, which start appearing about two weeks after infection, are not useful, Hanson said.
There are two other types: IgM antibodies appear later in SARS-CoV-2 infections than they do with other viruses, are less specific than IgG antibodies, and levels fluctuate more, she said.
IgA antibody tests do not effectively distinguish SARS-CoV-2 from other coronaviruses that cause common colds.
Even for population surveys, tests must be highly accurate, experts said. In populations with only a few people infected, even a 1% inaccuracy rate can introduce wide margins of error.
Antibody tests are different from antigen tests, which look for a protein on the surface of the virus. They are not considered highly accurate but give results in 15 minutes. Because laboratory backups and shortages of testing reagents have delayed more accurate PCR tests by as much as two weeks in some cities, many institutions have switched to using antigen tests.
Hanson said the society knew there was “a lot of interest” in antigen tests.
“But we have not even been able to get our hands on any to evaluate,” she said. “There are too many manufacturers with emergency-use authorization, and the demand is high.”
A positive result on an antigen test is generally considered accurate, she said, but a negative one means the patient should be retested with a PCR test.
Caliendo said her hospital in Rhode Island did not use antigen tests at all, and local schools used them to test only children who were clearly ill.
“We’re doing things that are less than ideal, because we can’t get the materials we need,” she added.
The society is looking at the new saliva tests, which appear to be about as sensitive as nasal swab tests, Hanson said, “but there’s not a lot of data on how long the virus is in saliva.”
Also, she said, “saliva is bubbly and hard to pipette.” As a result, labs are reporting 3% of tests invalid, compared to 1% for swab tests, “which is frustrating.”
On the other hand, she said, swabbing can make a patient sneeze, which endangers the person giving the tests. Spitting does not, Hanson said, “so you don’t need the same level of PPE — which matters, because here in Utah, it’s 100 degrees in the testing tents.”
First Published: Aug 24, 2020, 12:31
Subscribe Now