
Warning of shortages, researchers look to stretch vaccine supply
Scientists at the National Institutes of Health and drugmaker Moderna are analyzing data to see if they can double the supply of the company's coronavirus vaccine by cutting doses in half
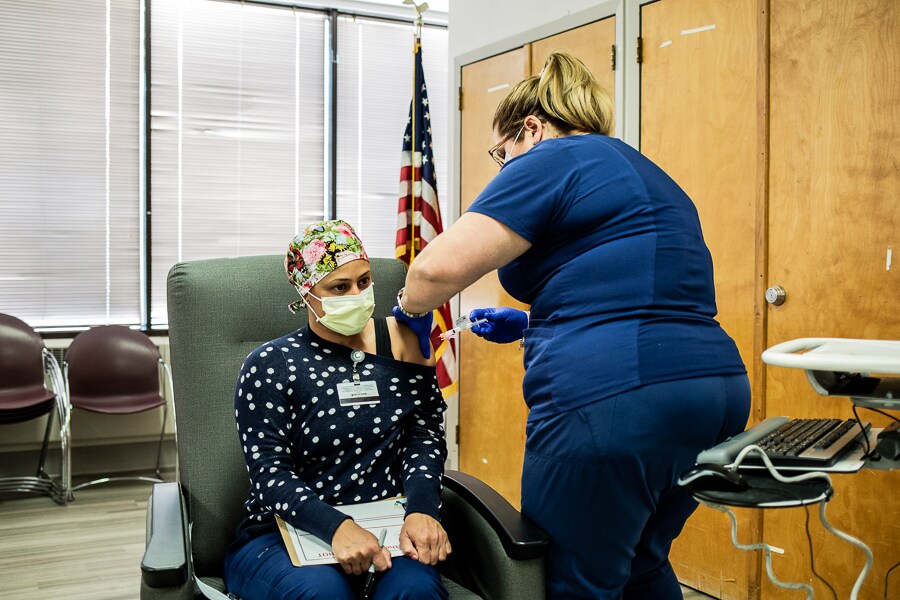 A health care worker receives one of the first doses of the Moderna COVID-19 vaccine, outside of a trial, at Christ Hospital in Jersey City, N.J., on Monday, Dec. 21, 2020. The NIH and Moderna are examining whether doses of Moderna’s coronavirus vaccine can be halved to double the supply, while scientists look for other ways to extend availability.
A health care worker receives one of the first doses of the Moderna COVID-19 vaccine, outside of a trial, at Christ Hospital in Jersey City, N.J., on Monday, Dec. 21, 2020. The NIH and Moderna are examining whether doses of Moderna’s coronavirus vaccine can be halved to double the supply, while scientists look for other ways to extend availability.
Image: Bryan Anselm/The New York Times
WASHINGTON — Federal officials and drugmakers, faced with a slower-than-expected rollout of the coronavirus vaccine, are racing to find ways to expand the supply, looking at lowering the required dosage and extracting more doses from the supplies they have.
Just weeks into the vaccine program, scientists at the National Institutes of Health and drugmaker Moderna are analyzing data to see if they can double the supply of the company’s coronavirus vaccine by cutting doses in half. The study, though long planned, is increasingly urgent in the face of looming shortages as the country tries to fight off a surging pandemic.
Officials are also rushing to find supplies of more efficient syringes that could extract an additional dose from vials of the Pfizer-BioNTech vaccine. That could bolster the Pfizer supply by 20%.
With more than 355,000 Americans already dead of COVID-19, nearly 21 million cases reported in the United States and hospitals overflowing, the need to inoculate people grows more urgent every day. The nation is facing twin problems. At the moment, it has only enough vaccine on order to cover 185 million Americans by the end of June. At the same time, doses that vaccine makers rushed out of their factories are sitting unused and are in danger of expiring.
The Trump administration has shipped more than 15 million vaccine doses, and millions more are already in the federal government’s hands. Yet only 4.5 million people have received them so far. State and local public health officials, already overwhelmed with rising infections, are struggling to administer the vaccine to hospital workers and at-risk older Americans while most people remain in the dark about when they might be protected.
©2019 New York Times News Service














