India's vaccine rollout: Cracking the bullwhip
A look at the knowns, the unknowns, and the strategies to avoid the biggest risks, including the dreaded supply chain in India's mass vaccination plan


The COVID-19 pandemic seems to be on a roller coaster ride in much of the western world. The new variants—in the UK, South Africa, Brazil—have exacerbated the already dire scenario. While the news is full of a grim winter in much of the US and the EU, India seems to have evaded the worst. However, the lull in India is tempered by a sense of uncertainty about mutations: some evade the natural immune response, some are transmitted more easily, and we now know that the UK variant causes a more severe disease, accompanied by a higher mortality. In all this gloom, the silver lining for India has been an abundant availability of vaccines. Even the UN Secretary General has praised India’s efforts of indigenously manufacturing vaccines. Yet, this reassurance must be tempered, given what we have seen of how the "Warp Speed" plan for vaccination in the US has unravelled. In this article, we highlight the knowns, the unknowns, and the strategies to avoid the biggest risks—including the dreaded supply chain bullwhip—in India’s mass vaccination plan.
The world’s largest vaccination drive
While India’s population is about 1.32 billion, those who are eligible for the vaccine—above the age of 18 —number at about 0.8 billion. According to Dr Anthony Fauci, a leader in the US anti-covid efforts, the entire population can only be assured with 85 percent to 90 percent vaccination rates. This implies that India needs to vaccinate 700 million people to achieve the famous "herd immunity". 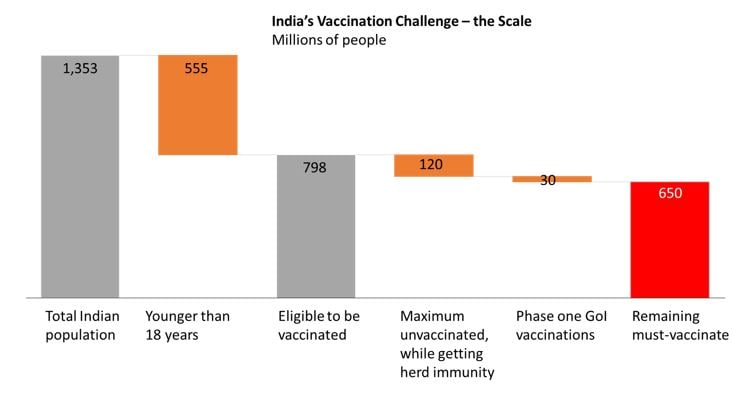 Since the summer of 2020, the government of India has been planning to meet the demand for vaccine development and distribution to stop the spread of Covid-19. The planning and now execution of the government’s vaccination plans essentially involve managing supply (input of vaccines into the national health system), managing demand (output, or getting eligible Indians the jab) and everything in-between—the logistics and distribution (throughput) to match supply with demand. The government has committed to vaccinating 30 million essential healthcare workers and frontline personnel in the first phase. The planning for this phase has involved multiple dimensions such as resource mobilisation, identification of vaccination centres, training of staff to administer the vaccine and dry runs.
Since the summer of 2020, the government of India has been planning to meet the demand for vaccine development and distribution to stop the spread of Covid-19. The planning and now execution of the government’s vaccination plans essentially involve managing supply (input of vaccines into the national health system), managing demand (output, or getting eligible Indians the jab) and everything in-between—the logistics and distribution (throughput) to match supply with demand. The government has committed to vaccinating 30 million essential healthcare workers and frontline personnel in the first phase. The planning for this phase has involved multiple dimensions such as resource mobilisation, identification of vaccination centres, training of staff to administer the vaccine and dry runs.
In execution, it is clear that the supply side is working, but demand management is mixed, largely driven by vaccine hesitancy. While states such as Uttar Pradesh and Odisha have achieved more than 70 percent of their vaccination targets, others such as Tamil Nadu and Punjab have reached only 20-30 percent of vaccination targets by end of week one. However, there has been a pick up in activity recently, and India has completed vaccinating four million people by the fourth week, the fastest in the world to reach this milestone.
Vaccine hesitancy, which was reported to be higher than 60 percent in India, in the first week of vaccination, has diminished with time as recipients are reassured of efficacy and safety. The bigger challenge lies beyond phase one—how does the government ensure access to vaccines for 650 million people, or 1.3 billion doses? This target is also time sensitive: health experts advocate 12-18 months for full vaccination, which implies a daily vaccination rate of 2.4-3.6 million. As public health is a concurrent budget item in India—both centre and the states are responsible—the central government is likely to pass on the responsibility for vaccinating much of the 650 million to state governments. While some states, such as Kerala and New Delhi, have vowed to offer free vaccination for all, other states are likely to take a stratified approach—subsidising distribution in government hospitals, but also allowing for private market distribution. This tiered system is more complex than that of the US, and it thus follows that India, is likely to experience similar supply-demand mismatches as the US: creating the dreaded bullwhip effect. Budget 2021 has made a provision of Rs 35,000 crores for vaccinating Indians, but the modalities are yet to be announced.
The Bullwhip and the Wave Method Strategy
The bullwhip effect describes a repeating cycle of acute demand overestimates, leading to spikes in supply, resulting in huge surpluses and waste, followed by demand underestimates, supply shortages, more demand overestimates, and so on. Parts of this bullwhip have already been observed in the US, with reports of states like Florida, having used only 50 percent of the vaccines delivered, while other states like Texas and Oregon are running out of stock. Given the decentralisation inherent in the multi-tier distribution—centre, state and private channels—India’s best bet would be to adopt a dynamic, demand-driven vaccine distribution approach: the "wave" method.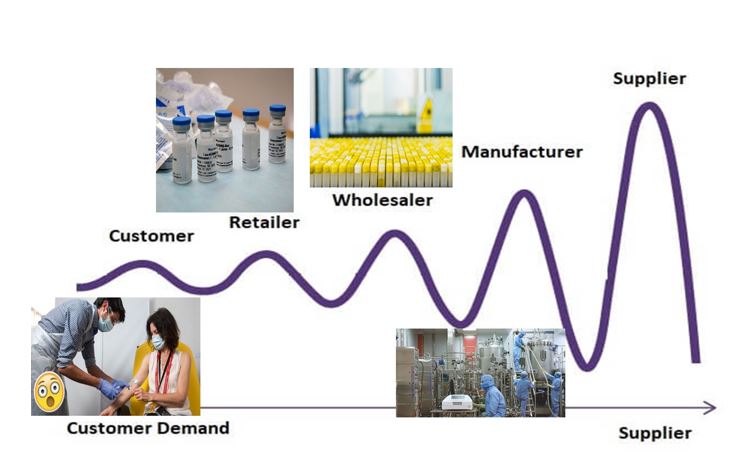 In phase one, 3,000 vaccination sites have been set up with a combined delivery capacity of 300,000 doses per day. To reach the required pace of 2.4-3.6 million doses per day in the following phases, India will need to ramp up its throughput capacity by 10X. And to avoid the bullwhip, the ramp-up needs to be dynamic: As certain regions demonstrate a spike in demand, distribution capacity to those outlets needs to be scaled up quickly, while also scaling down in regions where the demadn is waning. An ideal outcome would be one where the government could facilitate vaccination for 600 million Indians in 15 "waves" of vaccine jabbing, over 12 months. Thus, one wave would target 40 million persons that are vaccinated, using, say, 5,000 vaccine centres of appropriate size in regions with high need. In the second wave, the next 5,000 centres must be activated for the next 40 million, and so on.
In phase one, 3,000 vaccination sites have been set up with a combined delivery capacity of 300,000 doses per day. To reach the required pace of 2.4-3.6 million doses per day in the following phases, India will need to ramp up its throughput capacity by 10X. And to avoid the bullwhip, the ramp-up needs to be dynamic: As certain regions demonstrate a spike in demand, distribution capacity to those outlets needs to be scaled up quickly, while also scaling down in regions where the demadn is waning. An ideal outcome would be one where the government could facilitate vaccination for 600 million Indians in 15 "waves" of vaccine jabbing, over 12 months. Thus, one wave would target 40 million persons that are vaccinated, using, say, 5,000 vaccine centres of appropriate size in regions with high need. In the second wave, the next 5,000 centres must be activated for the next 40 million, and so on.
While the initial vaccine hesitancy might tempt some planners to reduce the number of centres, we recommend against it. Instead, the "wave" method will enable distribution to meet initial surges in demand, which can vary quite dramatically, once the strict constraints of phase one are removed, and virus mutations spread. As the wave method is dynamic, it can be ramped down rapidly in case of demand shortfall. The bigger challenge is execution, given the complex nexus of responsibility between states, the centre and private health distribution channels. We believe an important way to address this complexity is to invite India Inc to help with the rapid logistical and delivery scale up.
A Partnership between India Inc and the government
Companies such as Starbucks and Amazon—which have massive reach and logistical expertise—have offered both design and execution aid to the US government in vaccination logistics. Microsoft has offered to help in data analytics. In India, where the complexity is still greater, dynamic scaling up of throughput will need even more public-private partnership. This implies that the central government’s role will see a shift—from direct procurement and distribution in phase one, to an even more critical role of facilitation in the following phases. In managing demand, the government can further reduce vaccine hesitancy, (in fact, the government needs to create "vaccine urgency", although this should be done after ensuring that supplies are ready), e.g., through public service advertisements, including visuals of the prime minister, eligible chief ministers, and other prominent local leaders getting vaccinated. In supply management, the central government could aggregate cross-state demand to negotiate favourable prices. Another supply lever is fast-tracking the review of pipeline Covid-19 vaccines from the likes of Zydus Cadila, Dr. Reddy’s Lab, and others from the Serum Institute of India and Bharat Biotech. And in managing throughput, the data from the government’s CoWin app could be used by data science experts from India’s IT behemoths, to plan the locations and timings for vaccination ‘waves’. For only when states, the centre, and the private sector come together, can we win this deadly war.
By Malay Krishna - Professor and Chairperson, International Relations, Bhavan"s SPJIMR and R. Jayaraman - Head of Capstone Projects at Bhavan"s SPJIMR
First Published: Feb 11, 2021, 11:23
Subscribe Now