Is PM Modi's Ayushman Bharat too ambitious to succeed?
Inside India's health care fix: Fifteen months after Prime Minister Narendra Modi launched the Ayushman Bharat health scheme, stakeholders have mixed views


 Illustration: Sameer Pawar[br] On a humid afternoon last summer, Tasneem Sayed made her way to a student’s shanty in Kishanganj in northern Bihar, bordering West Bengal. The 26-year-old taught English and mathematics to Class 5 students while pursuing her BA alongside. “I returned home after tuitions that day and suddenly got high fever. I was totally fine until then,” she says, shrugging her slender shoulders.
Illustration: Sameer Pawar[br] On a humid afternoon last summer, Tasneem Sayed made her way to a student’s shanty in Kishanganj in northern Bihar, bordering West Bengal. The 26-year-old taught English and mathematics to Class 5 students while pursuing her BA alongside. “I returned home after tuitions that day and suddenly got high fever. I was totally fine until then,” she says, shrugging her slender shoulders.
When the fever didn’t subside, her father, a farmer, took her to the local hospital where she was diagnosed with jaundice. A sonography further revealed that she had a tumour, the size of two tennis balls, in her liver. “We were devastated when the doctors told us it was cancerous,” says Tasneem, whose identity has been changed on request.
On the doctor’s suggestion, Tasneem travelled to Mumbai for treatment at the Tata Memorial Hospital. Sitting on her bed in the female ward, arms wrapped around her bent legs, Tasneem wears a bubble-gum pink dupatta over her white hospital overalls. Her face is hollow-eyed and pale, but her high cheek bones and sharp nose cut a striking figure. Her surgery was successfully completed a few days ago, says her brother, Amir, who sits by her side.
“We received help through Ayushman,” he says measuredly, referring to Prime Minister Narendra Modi’s massive government-funded programme that promises health insurance to half a billion people. Dubbed ‘Modicare’, the scheme is built on two pillars: Establishing 150,000 primary health care centres to focus on prevention and early detection of diseases and providing a cashless cover of ₹5 lakh per family per year for secondary and tertiary care hospitalisation through the Pradhan Mantri Jan Arogya Yojana or PMJAY. Around 10 crore families or 50 crore people who make up the bottom 40 percent of India’s population as per the socioeconomic caste census data (SECC 2011) are eligible.
Since its launch in September 2018, six months ahead of the general elections, 71.69 lakh people have benefited from Ayushman Bharat-PMJAY, resulting in cost savings of ₹10,312 crore for them. Claims totalling ₹8,872.5 crore have been approved as of December 2019. “We have gained tremendous momentum in the first year,” says Dr Indu Bhushan, CEO of AB–PMJAY, in an interview at his New Delhi office.
*****
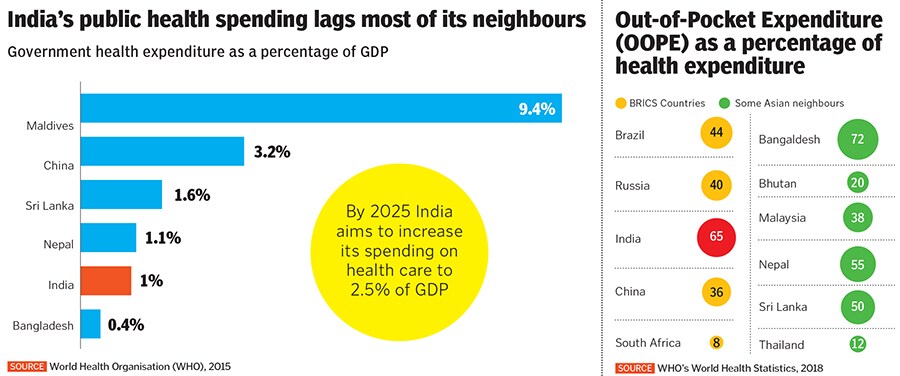
India’s public health record is abysmal. The government spends just about 1 percent of GDP on health care—one of the lowest levels in the world. The US, UK and China spend 8.5 percent, 7.9 percent and 3.2 percent respectively. Neighbouring countries Bhutan and Sri Lanka also score better, spending 2.5 percent and 1.6 percent, according to the World Health Organization.[br]Poor public spending on health has meant that access to free, quality health care at government-run hospitals is sparse. In search of better care, poor people wager their life’s savings, borrow money from informal lenders and sell assets to pay the bills. Out-of-pocket spending, which accounts for 65 percent of an individual’s health care expenditure in India, pushes 3 to 5 percent of the population into poverty, says the Public Health Foundation of India.
So to provide publicly funded health care to India’s poorest is a “game changer”, says Dr Devi Shetty, founder and chairman, Narayana Hrudayalaya Hospitals.
The premium for providing a ₹5 lakh annual medical cover to each family comes to around ₹1,100 and will cost around ₹12,000 crore in central and state government funds costs are to be borne by the Centre and states in a 60:40 ratio. When the late Arun Jaitley, as finance minister, had announced the scheme in his 2018 Budget speech, he called it the “world’s largest government-funded health care programme”.But the challenge lies in its implementation.
AB-PMJAY is an expansion of the central government’s Rashtriya Swasthya Bima Yojana (RSBY) which has an annual medical coverage of ₹30,000, and numerous other state government-funded health insurance schemes that have been running for several years. But these have had a patchy record. Several studies have reported no reduction in out-of-pocket expenses of those insured. One such study looking at hospitalisation cases based on National Sample Survey Office data found that for every 100 cases under various state government-funded health insurance schemes, only three got cashless treatment. This could be due to poor monitoring and improper regulatory regimes, write the authors.
“The government, health care providers and patients will have to go through teething troubles for the next year or so before things start running smoothly,” predicts Shetty, who has allocated 5 to 10 percent of beds at some Narayana Hrudayalaya hospitals for Ayushman Bharat patients.
***** The Tata Memorial Hospital in Mumbai charges 30-40 percent less for medical treatments compared to for-profit private hospitals
The Tata Memorial Hospital in Mumbai charges 30-40 percent less for medical treatments compared to for-profit private hospitals
Image: Mexy xavier[br]At Mumbai’s Tata Memorial Hospital, Amir pulls out a laminated, pink card from his shirt pocket. It’s Tasneem’s AB-PMJAY card, complete with a photo and fine print on the reverse detailing the services that can be availed of. “The government authorities came home to give this to us…. just months before I fell ill,” says Tasneem, smiling feebly.
Unlike RSBY, which required individuals to enrol themselves into the scheme at a particular time of the year, AB-PMJAY is an entitlement-based scheme. Cards have either been sent to eligible individuals based on the SECC 2011 data or they can approach an ‘Arogya mitra’ stationed at every empanelled hospital to get a card made on the spot. “This is a considerable difference between the two schemes and one that is less exclusionary for a patient seeking care,” says Dr Indranil Mukhopadhyay, health economist and associate professor at OP Jindal University, in Haryana.
Another difference between the two schemes is that states are given the flexibility to implement AB-PMJAY in the way they like. They can opt for an insurance-based model, deploying an insurance company to handle the claims or they can go with a trust model where the state government handles the claims. Of the 33 states and Union Territories that have taken up the scheme—Delhi, Telangana, Odisha and West Bengal are not yet on board—a handful have opted for a mixed model, combining the best of the insurance and trust models. Some states like Karnataka and Kerala, which had seven and three state health insurance schemes in place respectively, are in the process of subsuming them under AB-PMJAY, says Bhushan. Others like Maharashtra, which runs the Mahatma Jyotiba Phule Jan Arogya Yojana (MPJAY) health insurance scheme (previously known as the Rajiv Gandhi Jeevandayee Arogya Yojana), is implementing AB-PMJAY as a parallel scheme. The former has a medical cover of ₹1.5 lakh. Once that amount is used, then only can patients dip into the additional ₹5 lakh offered under AB-PMJAY.
In Bihar, Tasneem and Amir’s home state, no state health insurance scheme existed prior to AB-PMJAY. “We are lucky,” says 30-year-old Amir. He left Kishanganj a few years ago to settle in Mumbai where he teaches Arabic at a madrassa. It pays him ₹6,000 a month. He rents a room in a chawl in Malad and gives tuitions to supplement his income. “I end up earning a total of ₹10,000 to ₹15,000 a month. Without this,” he says, holding up the pink card, “we would not have come so far.” Tasneem, still hunched over her bed, nods in agreement.
***** In 2018, the government allocated ₹1,200 crore to the primary health care pillar of Ayushman Bharat and ₹2,000 crore to insurance pillar, PMJAY. The following year, the latter was ramped up to ₹6,400 crore.
In 2018, the government allocated ₹1,200 crore to the primary health care pillar of Ayushman Bharat and ₹2,000 crore to insurance pillar, PMJAY. The following year, the latter was ramped up to ₹6,400 crore.
“I am not suggesting that the scheme needs more money… I am saying the insurance model is inherently a cost escalating one,” says the professor. RSBY, with its ₹30,000 coverage, for instance, had a premium ranging from ₹350 to ₹900, with the amount increasing every year. With PMJAY too, as the number of claims increase, premium prices—currently at around ₹1,100—will shoot up. Reimbursements demanded by hospitals will consequently increase.
However, Bhushan bets that as the number of claims increases, the marginal costing of hospitals will decrease. “Eventually we want hospitals to move to a high volume, low margin model,” he says.
Hospital executives tend to disagree. “You can’t run hospitals like factories,” says the head of one leading private hospital chain on the condition of anonymity. “Doctors and nurses are human and can only work so many hours in a day. The whole ‘economies of scale’ argument just doesn’t work in the health care sector.”
AB-PMJAY currently covers 1,393 medical procedures, and the package rates for them are between 40 percent and 80 percent lower than what private players charge. Months after the scheme was launched, the Association of Healthcare Providers, a not-for-profit body that represents the majority of health care providers in India, wrote a letter to the authorities requesting for a revision in package rates. The letter noted that the prices were “unscientific” and “insufficient”.
Prices have since been revised the government brought on board the Post Graduate Institute of Medical Education and Research, Chandigarh to come up with more suitable rates. But private players are still unhappy.
*****
To combat Tasneem’s liver cancer, doctors at the Tata Memorial Hospital first gave her transarterial chemoembolisation (TACE) injections thrice, at weekly intervals. Containing anti-cancer drugs, the injections helped destroy some of the cancer cells and also reduced the supply of blood to the tumour, starving it of the nutrients it needs to grow. “The injections helped shrink the tumour,” says Amir.
AB-PMJAY covered the entire ₹1 lakh cost of the treatment. “I didn’t have to pay anything,” he says. He just had to show his sister’s card and medical file at the AB-PMJAY counter at the hospital the authorities keyed the data into their computers and gave the Sayeds the benefit of cashless treatment.
Often, surgery can be avoided after TACE injections, but in Tasneem’s case, it was necessary. She was successfully operated upon, but this time the ₹1 lakh-plus bill that was clocked up could not be covered by AB-PMJAY because the package amount was exhausted. “I showed them her card at the counter after the surgery, they checked their computer and said I will only get ₹10,000 now,” says Amir. Tasneem winces in pain as he speaks, pressing her forearm to her upper-right abdomen, just under her ribs. “I feel a shooting pain on and off,” she says softly.
Amir managed to get the balance amount from a trust that specifically helps patients from Bihar, but the expenses are spiralling. “The hospital stay, the tests, drugs, transportation, it’s all adding up,” says Amir. “They say it’s a ₹5 lakh cover, but you don’t get that amount. I understand they have their limits per treatment, but her treatment is not yet done.”
*****Profit margins of listed hospital chains are 15 percent to 20 percent at best. If the discount between our prices [for medical treatments] and Ayushman Bharat’s listed prices is more than 15 percent, we’ll go at a loss,” says the chairman of a top hospital chain that has chosen not to be part of AB-PMJAY.
He breaks down the economics of a hospital: Say the cost of a surgical procedure is ₹100. Doctor fees, direct consumables and medicines cost about ₹50 on average. Thereafter around ₹35 gets consumed by other costs such as staff salaries, administration costs, electricity, power, stationary etc. That leaves an operating profit of ₹15.
“Your interest and loan repayments are made from the ₹15 what’s left thereafter is your cash flow. That is the construct of a hospital business,” he says dryly.
“Now if the market price is ₹100, the Ayushman Bharat price is close to ₹30. But let’s say, it’s ₹50. How can we do this? It’s totally unviable. If anyone can do this, they should have 50 percent margins.”
Forbes India interviewed more than 20 C-suite executives, doctors and technicians working at private hospitals in metros and smaller towns, most of whom spoke off the record. They were unanimous in their view: AB-PMJAY is noble in intent and they’d like to play a role is offering quality health care to the less privileged, but at the present package rates, it is unfeasible.
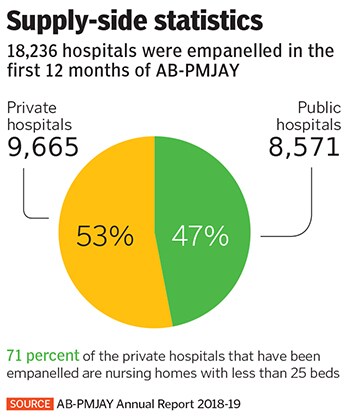
So which hospitals are carrying out procedures under AB-PMJAY? According to official data, 53 percent of the 46.5 lakh treatments completed as of September 2019 have been carried out by private players. Since most of the large private hospitals have stayed away from the scheme—notable exceptions are Apollo which has allocated about 5 percent of its bed capacity in tier 2 and 3 towns for AB-PMJAY patients and Narayana Hruduyalaya—what’s left are smaller hospitals and nursing homes. According to AB-PMJAY’s 2018-19 annual report, of the 53 percent treatments carried out by private players, 71 percent were done at hospitals with less than 25 beds.
“Packages are unrealistic,” says Dr Shailesh Shrikhande, head, division of cancer surgery and deputy director, Tata Memorial Hospital. “We are in a privileged position because our costs are anyway 30 to 40 percent less than what a [for-profit] private hospital would charge because of bulk buying of drugs and equipment. We also receive a subsidy from the Department of Atomic Energy [because of the radiation technology used in treatment],” he explains. Tata Memorial treated 1,183 patients under the AB-PMJAY scheme between January and November 2019 48 percent of those claims have been settled.
Take, for instance, a surgery to treat pancreatic cancer or Whipples as it’s known in medical parlance. It is widely regarded as one of the most complex operations, says Shrikhande, referring to his area of specialisation. Without complications, such a surgery costs around ₹1-1.5 lakh at the Tata Memorial Hospital. A for-profit private hospital would charge between ₹3 lakh and ₹15 lakh for the same procedure. Government hospital rates tend to be about six times lower, according to a recent pan-India study by the Union Ministry of Statistics and Programme Implementation.
Ayushman Bharat offers a measly ₹25,000 package. “This is a clear reflection that detailed homework has really not been done,” says Shrikhande, adding that the Whipples package offered by the Maharashtra government-funded MPJAY is much higher at ₹75,000. The latter, he says, is “not bad” as one can cross-subsidise the balance amount from full-fee paying patients. However, patients might still have to resort to catastrophic out-of-pocket expenditure, he cautions.
Add complications into the mix, which happen in 30 percent of the cases, he estimates, and the economics just don’t work.
“You can’t expect Shiv Sagar rates at JW Marriott,” says one private hospital executive.
“I’ve been told by officials that they don’t really want hospitals from metros to come on board the scheme,” says another head of a group of hospitals. “They’re looking at hospitals in tier 2 and 3 cities. Even then, I don’t think the math works out.”
“It’s a myth that these rates are viable in tier 2 and 3 city hospitals,” says a doctor-cum-promoter of a hospital chain in interior Maharashtra. “Staff costs might be lower here, but it’s still loss-making for us to treat patients at these rates.”
To incentivise large hospitals to set up shop in smaller towns, AB-PMJAY is offering land at subsidised rates and also “viability gap funding” to support infrastructure building. “We are considering such an option… the success of the scheme relies on participation from the private sector,” says Dr Ashok Seth, chairman of Fortis Escorts Heart Institute.
*****
Knee surgeries grew in popularity when the procedure was included in the Gujarat government’s Mukhyamantri Amrutum health insurance scheme launched in 2012. “Private players were cooking up patients, doing unnecessary surgeries just to claim the reimbursement,” recounts the head of a Gujarat-based chain of hospitals on the condition of anonymity.“One day we got an X-ray with the patient’s name scratched out for checking. Our doctors examined it and said no surgery was required,” he recalls. “We were later told that a knee surgery had already been performed on that patient… the government authorities debarred that hospital.” Herein lies the flip side of increasing package rates too much and too fast—private players are tempted to profit from the scheme. The AB-PMJAY authorities, he says, are equally vigilant. “They have spent lots of time with our team here to understand the challenges in implementation.” Meanwhile, artificial intelligence and machine learning are being used to catch abnormalities in patient data and take corrective action if needed, says AB-PMJAY’s Bhushan.
“It is, of course, a drain on the exchequer to keep increasing the package rates. That’s understandable,” says Abhay Soi, chairman of Radiant Life Care, which acquired Max Healthcare in December 2018.
Tiered pricing for different hospitals based on geography, hospital accreditation and patient outcomes is one solution. “Rates can’t be the same for an angioplasty done in a tier 2 city hospital and one done at AIIMS or Escorts,” explains Seth.
Co-payment could be considered where patients contribute say ₹10 to the scheme every month, says Shrikhande of Tata Memorial Hospital. “This will increase the pool of money available.” In fact, the next stage of AB-PMJAY, says Apollo Hospitals’ Suneeta Reddy, must include India’s middle class. “If the average Indian can spend ₹500 on a digital plan for their phones, an amount similar to it is well worth it for good health,” she says.
“The entire model needs to be re-thought,” says Soi. “If the government can reverse auction land in metros for volunteering maximum beds to Ayushman Bharat, large FDI can be attracted for creating infrastructure. We can then treat Ayushman Bharat patients as well as other [full-fee- paying] patients. That is a viable model.”
Finally, strengthening primary care is imperative. The 150,000 “health and wellness centres” that form the first pillar of Ayushman Bharat are an “investment for the future”, says Mukhopadhyay of OP Jindal University. With the focus on prevention and early detection of diseases, especially non-communicable diseases (NCDs), these centres in the long run will protect people from falling severely ill and reduce the burden on secondary and tertiary care hospitals. According to official data, almost 20,000 such centres were fully functioning as of July 2019. “Much more resources are needed [₹1,200 crore has been allocated thus far] to fully equip these centres with the right infrastructure and manpower. The insurance scheme with its escalating costs diverts funds away from this,” adds Mukhopadhyay.
*****
Amir hops off the train at Mumbai"s Parel station with a heavy knapsack slung on one shoulder, and weaves his way to the Tata Memorial Hospital. He has to take an appointment for his sister’s next visit with the doctor. She was discharged a week earlier. Dressed in a white kurta and a skull cap, Amir completed his morning classes at the madrassa and got here. “Can’t it be done over the phone?” Forbes India asks. “It can,” he says haltingly, “but it’s much quicker if you come here and do it. Takes just 10 minutes.” But he quickly adds, “Of course it’s troublesome coming all the way from Malad, but it’s for my sister.”
As he waits in queue for his turn, he swings his knapsack towards his chest and pulls out Tasneem’s file. He points to an ID number on the front. “They need this to give me the appointment,” he explains. Soon enough Tasneem will have to start radiation and chemotherapy. Ayushman Bharat will cover some of the cost, but not all of it. Amir opens the file and shows copies of the letters he has sent to different charitable organisations asking for monetary help. “Once she’s done with all this, I’d like her to do a nursing course. And then get some practical training at a hospital. I want her to be independent,” he says.
Can Ayushman Bharat truly reduce the burden of health care costs on poor families? “I had no hope that we would come even this far with Tasneem’s treatment. But look where we are,” says Amir. “We’ll take one step at a time, Mashallah. Something will work out.”
Also read: "The private sector will never be happy": Ayushman Bharat CEO Dr Indu Bhushan
First Published: Jan 23, 2020, 09:13
Subscribe Now