MHI seeds the Alliance for Suicide Prevention in India that collaborates with organisations, activists, funders, researchers and policymakers to prevent suicides at individual and community levels. As per the latest available statistics from the National Crime Records Bureau (NCRB), 164,033 people died by suicide in 2021, a 7.2 percent increase from 2020. Collecting data around suicide requires understanding of the context, ensuring affected people have access to helplines or other support, and respecting their right to privacy, Mariwala explains. “There is a need to have a public health approach which looks at data carefully, leverages community resources, has inter-sectoral collaboration and uses data to design prevention solutions," he says.
There is a lot to unpack here. About how supporting people with mental health issues needs to leverage community help, how it takes different stakeholders to do their part and work together, how they all need to work with sensitivity and empathy. And treating mental health as health is the starting point of all this.
Mariwala is among a handful of businesspersons who has been dedicatedly working to improve people’s access to mental health services through MHI. A few other philanthropists and organisations who have been supporting mental health causes at scale include Wipro Chairman Azim Premji, Biocon CMD Kiran Mazumdar-Shaw, Tata Trusts and Aditya Birla Education Trust.
The last quarter saw two other prominent philanthropists bolster their support towards causes related to mental health. In February, the Indian Institute of Science (IISc) said it will receive Rs450 crore from Infosys co-founder Kris Gopalakrishnan for their Centre for Brain Research that will specifically carry out deep science research on neurodegenerative diseases, which can impact a person’s mental health and wellbeing, and people might require mental health support alongside medical treatment.
In March-end, Rohini Nilekani, through Rohini Nilekani Philanthropies (RNP), announced a grant of Rs100 crore over the next five years to the National Institute for Mental Health and Neurosciences (NIMHANS) and the National Centre for Biological Sciences (NCBS) to establish a centre for brain and mind, which will work towards enabling long-term research and practice on schizophrenia, bipolar disorder, obsessive-compulsive disorder, dementia and addiction.
Nilekani says she took her time to find the right partners to support institutional giving at scale. In 2017, she had backed a report along with Ashoka: Innovators for the Public to study the mental health landscape in India. Since then, she made small grants to non-profits working in this space, but nothing very large or significant. “It is a very hard space to be effective in at the scale required. Because the problem itself is so large," she says.
Why is Philanthropic Funding Low?
Nilekani is right about the problem being a very large one. The National Mental Health Survey (NMHS) 2015-2016 says that nearly 80 percent people struggling with mental health illnesses in India were not seeking and receiving care. The treatment gap for common mental health disorders (like depression, suicidal behaviour, substance use problems) was 85.2 percent. It was 75.5 percent for psychoses, 70.4 percent for bipolar affective disorders and 86.3 percent for alcohol use disorder.
An article in The Lancet titled ‘The burden of mental disorders across states of India: The global burden of disease study 1990-2017’ said one in seven Indians was affected by mental disorders of varying severity, and that the proportional contribution of mental disorders to the total disease burden in India had almost doubled since 1990. The article—which was published in December 2019, and funded by the Bill and Melinda Gates Foundation, Indian Council of Medical Research, and Ministry of Health and Welfare, Government of India—said that in 2017, 197.3 million, or 97 percent Indians, had mental disorders in India, with 45.7 million with depressive disorders and 44.9 million with anxiety disorders.
The ‘Global prevalence and burden of depressive and anxiety disorders in 204 countries and territories in 2020 due to the Covid-19 pandemic’ study, published in October 2021 in The Lancet, estimated an increase of about 35 percent in the prevalence of anxiety and depression in India during the Covid-19 pandemic.
There is no recent government data of the scale of the NMHS available. Vikram Patel, professor at the Department of Global Health and Social Medicine at Harvard Medical School, says that while Covid-19 could have introduced a different disease burden pattern for a while, the last published data on mental health in India would probably be very similar going forward. “If you look at the relative health burden, the slice of the pie for mental health is growing," he says.
![]()
According to him, there are two demographic risk groups: Young adults and senior citizens. “Mental health problems predominantly arise during young adulthood, so while India’s youth population keeps increasing as a relative share of total population, which it will over the next few decades, we’re going to see a continuous increase in the relative burden of mental health problems," he says.
India will also have an ageing population, he adds, and among that group the risk is high of neurological diseases like dementia. “As a health care system, we are completely unprepared for either," says Patel, who is the co-founder of non-profit Sangath that works in the mental health space.
There’s very little support for mental health from Indian philanthropy despite the scale of the problem, because philanthropists have traditionally focussed on issues with high mortality and basic health care delivery for rural and low-income populations, which is also very important. So even though health care ranks second-highest in priorities for Indian philanthropists after education, there is no data available for how much of it goes towards mental health. It is likely to be miniscule, which would be in line with global trends as well, where philanthropic funding towards mental health, studied between 2015 and 2018, was less than 1.3 percent, according to data from the Center for High Impact Philanthropy in the US.
![]()
The reasons for low philanthropic funding towards mental health are a result of both demand and supply-side factors apart from existing cultural biases, says Pritha Venkatachalam, partner and co-head, Asia and Africa, The Bridgespan Group, which offers advisory and knowledge services to philanthropies, impact investors and non-profits. On the demand side, she says, people do not seek help for mental health issues due to low awareness, stigma, fear of ostracisation and other cultural factors. In many cases, cost of therapy or counselling is prohibitively expensive. “To most Indians, not being able to afford care is part of the treatment gap. Then there are geography- and gender-based barriers as well," she says, adding that on the supply side, India has a shortage of both mental health professionals and non-profits who could implement mental health initiatives at scale.
![]()
An April 2019 article published in the Indian Journal of Psychiatry estimated that India had 9,000 psychiatrists, 2,000 psychiatric nurses, 1,000 clinical psychologists, and 1,000 psychiatric social workers. To reach the median requirement of three mental health professionals per one lakh population, India would need an additional 30,000 psychiatrists, 37,000 psychiatric nurses, 38,000 psychiatric social workers and 38,000 clinical psychologists. “As per the calculations, it will take 42 years to meet the requirement for psychiatrists, 74 years for psychiatric nurses, 76 years for psychiatric social workers, and 76 years for clinical psychologists, for providing care for 130 crore population," the study says.
The paucity of trained talent is also in turn likely to pose a challenge to philanthropists who seek to large-scale research or programmes in mental health. While government interventions have to do most of the heavy-lifting, there might be scope to use philanthropic financing for capacity-building.
Venkatachalam, who believes that the Covid-19 pandemic helped turn people’s attention towards the need to support mental health causes, breaks down the value chain into various buckets. There is awareness generation and behaviour change, there is counselling and access to medical care, there is building capacities of mental health workers, providing local support, setting up community groups and providing training opportunities.
“Most philanthropic funding is on the initial end of the spectrum—awareness generation, behaviour change communication, counselling and access to medical care. But there is not too much on providing training for building capacity or rights-based interventions that help with legal aid or create awareness about the rights of mentally challenged individuals," she says.
More philanthropists must take the effort to have a systems-based funding approach, says Bhairavi Prakash, founder of Mithra Trust, a non-profit that provides access to groups and communities to help people discuss mental health challenges. Prakash needs at least Rs10-12 lakh annually to run each programme. She says that even though they got some funding in the immediate wake of the Covid-19 pandemic, as a lot of individuals and companies started paying attention to mental health, “many of those projects seem to have disappeared".
Many-a-times, there have been requests from donors to change their approach, and maybe just get funded to teach mental health at schools they support. “So, while addressing gaps, I think the biggest issue is lack of a systems approach." This means, according to Prakash, acknowledging that mental health care as part of health care, and not necessarily go after “quantifiable results".
Nilekani calls her funding risk capital that is sorely needed for long-term impact. “For the project that we have undertaken with NIMHANS and NCBS, we don’t know what will come out, but the research itself will be open source to other researchers across the world to build on," she says. For me, that is an important way to continue the innovation chain. “You need to be patient."
![]()
Mariwala also agrees that significant funding in India seems to go to tertiary mental health, such as mental health institutions, research and awareness campaigns. The funds go towards either breaking the stigma or understanding how the brain impacts mental illness. “This implies that we are asking people to talk about mental health, but there is no service delivery once they decide to speak up," he says. “We are also seeing a lot of interest in funding towards mobile apps for support, but in a country where a large number of people live below the poverty line, where illiteracy is high and English is not the language for communication, this modality of service delivery seems counter-intuitive."
He believes that most philanthropists are advised on mental health by psychiatrists or psychologists, which explains the current flow of funding. “Also probably, most philanthropists are using the same yardsticks for mental health as they use for business," he says, adding that just like in business, it would help them to understand the demand, and speak with the users of mental health services to understand their challenges, the price point at which they are willing to access services, and given the stigma around mental health, where would they be willing to access it from. “
Watch: "Philanthropy is a term unfortunately reserved for those who write big cheques": Amit Chandra
According to him, philanthropic funding should be prioritised for “service delivery, working on mental health of specific vulnerable groups, research on local models of support, and of course, advocacy with the government".
Samaj, Sarkar, Bazaar
The relationship between policy and philanthropy is mutual, says Patel of Harvard Medical School, so there’s no question that when the government says that a particular issue is of importance to itself, philanthropists will follow. Every stakeholder has a role to play and each of them is interconnected, he says. “The role of philanthropy is to promote innovations aligned with community and pilot scale ups that demonstrate how new discoveries and approaches can be delivered in real world settings outside the research context. But the role of ultimate scale up and wider adoption is going to always be that of the government," he says, adding that he has already started seeing a positive shift from both policy and philanthropy perspectives.
Neerja Birla, founder and chairperson of mental health organisation Mpower, has been seeing more philanthropists in her network support research and help non-profits improve access to quality care. The challenge to high-impact funding, according to her, comes with them requiring ‘demonstrable immediate and measurable outcomes’, which is very difficult in mental health. But her conversations with philanthropists, more and more, have started to revolve around how to improve longer-term funding at low costs, innovate partnership models inclusive of the local context, and emphasise on community-based care with institutional support. “These discussions demonstrate a growing recognition of the importance of mental health and a collective effort to address the issue," she says, over email.
Venkatachalam agrees that the examples of the Mariwalas or Gopalakrishnan or Nilekani supporting mental health causes with both their money, network and efforts will set a positive example for others to follow.
In order to remove the stigma associated with mental health, it is important to change the health care delivery itself, Patel says. This means moving away from asylum-centric care that excludes, sedates and keeps you away from your people, to a community-driven approach where you have mental health care services being provided by primary health care and frontline workers.
India brought out the National Mental Health Policy in 2014, which was followed by the Mental Healthcare Act in 2017. Various other initiatives were started in the wake of the Covid-19 pandemic, including the national telemental health programme that was announced in Budget 2022, telemedicine consultations through the e-Sanjeevani program, and the National Suicide Prevention Strategy that was launched by the health ministry in November 2022.
![]()
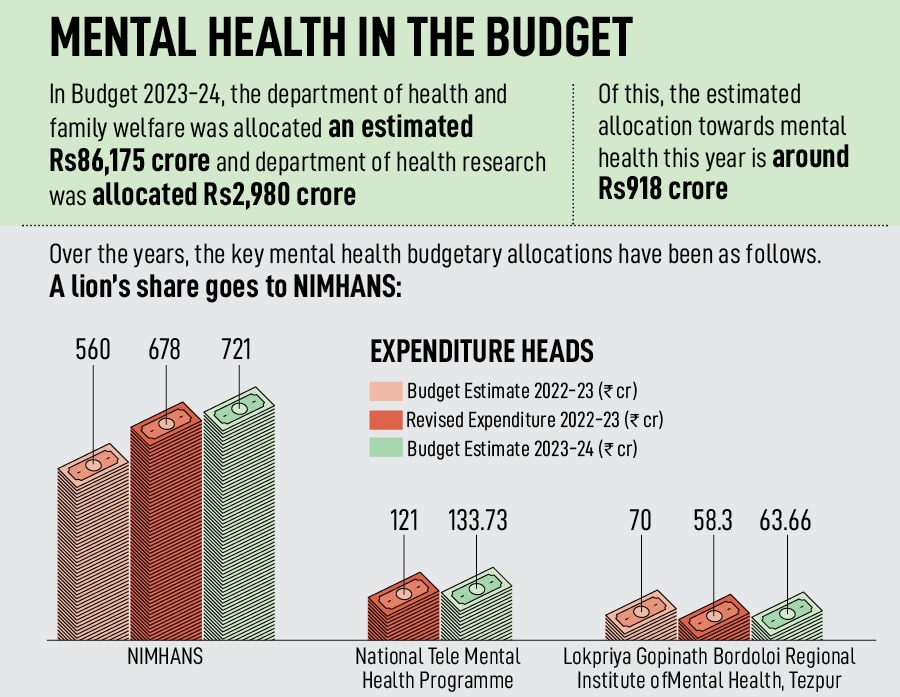
A large share of the Budgetary allocation towards mental health goes towards two centrally-funded institutions. While NIMHANS received an estimated allocation of Rs721 crore in Budget 2023, the Lokopriya Gopinath Bordoloi Regional Institute of Mental Health in Tejpur received an estimated Rs64 crore. The national tele-mental health programme has been allocated Rs134 crore. Not much is known about how all these programmes and funds will be implemented and utilised respectively.
Nilekani believes that India has seen some fairly progressive laws in the mental health space over the past few years, but the government has to do more both at the Union and state level by supporting both research and therapies, and creating treatment capacity right from the primary health care centre levels. “Diagnosis is key if we have to engage with people and help them with their right to seek treatment. So, training people at the first tier of the health care system as to how to identify or diagnose in an empathetic manner without shaming or judging is critical."
As far as the role of philanthropy goes, she hopes that the work she and her peers are doing will help signal that mental health is a space where a lot more people from philanthropy need to come in. “It doesn’t matter if they are small, medium-sized or large grants, but we need a lot more people to feel comfortable in supporting research and capacity-building, for mental health at all levels."