It's not just Maiden Pharmaceuticals. India's health care authorities also need
Experts say lax inspection and certification processes mean substandard products by repeat offenders are allowed to be sold in domestic and export markets


Up until October 5, New Delhi-headquartered Maiden Pharmaceuticals was having a relatively good run in the $25 billion pharmaceutical export market.
Maiden’s products were sold across the world, from Chile and Venezuela in the Latin American markets, to Senegal and Burkina Faso in Africa, and Vietnam and Cambodia in Southeast Asia. In all, according to the company’s website, its products are sold in over 41 countries.
On October 5, however, that dream run of 32 years came to a halt. The company is being accused of selling contaminated products that have been potentially linked to acute kidney injuries and 66 deaths among children in the Gambia, according to World Health Organization (WHO).
The four medicines are cough and cold syrups produced by Maiden: Promethazine Oral Solution, Kofexmalin Baby Cough Syrup, Makoff Baby Cough Syrup, and Magrip N Cold Syrup. According to WHO, the company hasn’t to date provided guarantees to WHO on the safety and quality of the products.
Laboratory analysis of samples of each of the four Maiden products has confirmed, according to WHO, that they contain unacceptable amounts of diethylene glycol (DEG) and ethylene glycol as contaminants WHO also reckons the products may have been sold outside of the Gambia.
“Diethylene glycol and ethylene glycol are toxic to humans when consumed and can prove fatal," WHO said in a report. “Toxic effects can include abdominal pain, vomiting, diarrhoea, inability to pass urine, headache, altered mental state, and acute kidney injury which may lead to death. All batches of these products should be considered unsafe until they can be analysed by the relevant National Regulatory Authorities." In 2020, some 14 children died in Himachal Pradesh due to the same contaminants—diethylene glycol—after consuming cough syrup made by another Indian company.
Maiden Pharmaceuticals, which has now been suspended by the pharma exporters’ body, Pharmexcil, however, refuted the allegations. “We are shocked to hear the media reports regarding the deaths and deeply saddened on this incident but we received the official information from our agent at the Gambia on 5th October 2022 and on the subsequent date, World Health Organization alert was issued against us," the company said in a statement.
India’s government agencies have since visited the company’s factories on four occasions and samples were drawn by the The Central Drugs Standard Control Organisation (CDSCO), which is responsible for approval of new drugs, conduct of clinical trials, laying down the standards for drugs, quality control of imported drugs and coordination between state drug control organisations. “We are awaiting the results and since the matter is already pending investigation and is subjudice, we cannot comment on any other issues," the company said in a press statement. Maiden is yet to respond to a questionnaire from Forbes India.
Headquartered in Pitampura in New Delhi, Maiden Pharmaceuticals was set up in November 1990.
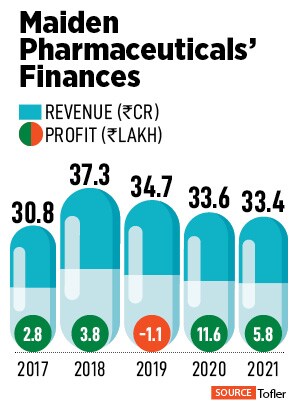
The company’s manufacturing units in Panipat and Kundli in Haryana are capable of manufacturing 600 million capsules, 18 million injections, 0.3 million tubes of ointments, 2.2 million units of syrups, and 1,200 million tablets annually. The company manufactures everything from lifesaving drugs to antibiotics. “Our sincere efforts of practicing and providing high-quality products are recognised by national and international certifying agencies and have honoured us with ISO 9001:2000 and WHO GMP certificate," Maiden claims on its website. The company has three directors, Vinod Kumar, Naresh Kumar Goyal, and Vivek Goyal. As of March 2021, it had revenues of Rs 38 crore, while its net profits stood at Rs 5 lakh.
On October 8, the company went on to refute the allegations made against it, following reports of the deaths in the Gambia. “We have valid drug approvals for the export of the products in question and we are not selling anything in the domestic market, so it is for export only," the company said in the statement. “We have been obtaining the raw materials from certified and reputed companies"
This isn’t the first time that Maiden Pharmaceuticals have been pulled up for manufacturing substandard drugs. According to data from the Xtended Licensing and Laboratory Node, a government-owned database, the company had been pulled up at least five times in Kerala alone in the past few years for substandard tablets. Apart from Kerala, it was also blacklisted by the Bihar government in 2011.
In 2014, Maiden was among 66 other Indian companies blacklisted by the Vietnam government for violating Quality Control Regulations and Drug Regulations. India’s Consul general in Vietnam, Deepak Mittal had then written to India’s Ministry of Health and Family Welfare (MoHFW). “It is requested that necessary background checks on these companies may kindly be undertaken in India to see if there are complaints from other countries and steps be initiated to penalise them for bringing bad name to the Indian pharma industries abroad," Mittal’s letter said, according to RTI documents issued to lawyer Prashant Reddy.
Yet, the CDSCO issued a Certificate of Pharmaceutical Products (CoPP), as mandated by WHO, to Maiden. Drug makers need a CoPP to manufacture and export a product, as it provides assurance that a plant complies with the minimum standards of procedure and production as prescribed by WHO.
“If the company had followed GMPs, it would have tested the excipients before using them in formulation and would have detected the DEG contamination before releasing its product to the market," says Prashant Reddy T and Dinesh Thakur, co-authors of the upcoming book The Truth Pill: The Myth of Drug Regulation in India. “It very likely did not test the excipients, but we need to see the final investigation reports to establish this. This is a tragedy that could have been easily avoided. What worries us is that neither the Ministry of Health nor the industry have learned their lessons from the five earlier DEG mass poisoning incidents in India."
 India has had a tumultuous history with DEG. Apart from the 12 children who died due to DEG poisoning in 2020, some 36 deaths were reported in Gurugram in 1998. Back then, too, children aged between 2 and 6 had died due to renal failure after consuming cough syrups made by a local manufacturer, according to news reports. Other instances include the death of 14 people in Mumbai in 1986 from DEG poisoning. In the US, the Federal Food, Drug, and Cosmetic Act was passed as a reaction to the death of 105 people who died from diethylene glycol poisoning in 1938.
India has had a tumultuous history with DEG. Apart from the 12 children who died due to DEG poisoning in 2020, some 36 deaths were reported in Gurugram in 1998. Back then, too, children aged between 2 and 6 had died due to renal failure after consuming cough syrups made by a local manufacturer, according to news reports. Other instances include the death of 14 people in Mumbai in 1986 from DEG poisoning. In the US, the Federal Food, Drug, and Cosmetic Act was passed as a reaction to the death of 105 people who died from diethylene glycol poisoning in 1938.
On its part, the government has shifted the blame to importing countries for ensuring the quality of the products sold from India. “It is a usual practice that the importing country tests these imported products on quality parameters, and satisfies itself as to the quality of the products before the importing country decides to release such products for usage in the country," the MoHFW said in a statement. The government also added that the cough syrups were never sold domestically.
“Well, the company that stands accused of this current fiasco in the Gambia is on the CoPP list put out by the CDSCO meaning that the CDSCO was certifying its products for export," Thakur says. “So yes, it does bear some responsibility for this fiasco. Prashant and I had to write a whole book about this topic. Clearly, we have serious misgivings about the nature, structure, and accountability of the drug regulator, CDSCO."
India’s pharmaceutical industry is pegged to be the third largest in the world by volume, worth some $40 billion. The country’s pharmaceutical sector exports to over 200 countries, and accounts for 3.5 percent of the total drugs and medicines exported globally. The country currently has the second-highest number of USFDA-approved plants outside the US and accounts for 60 percent of global vaccine production.
“We don’t think there exists any problem for the pharmaceutical industry to secure licenses, approvals, or any kind of clearance at the state level," Thakur and Reddy add. “In fact, our research tells us that most states turn a blind eye toward even flagrant violations because they are more interested in the licensing revenue that the industry provides for their coffers. The problem is transparency at the level of regulatory clearances. Indian law requires every manufacturing facility to be inspected annually for GMP compliance but we never see the reports from these inspections. Ask yourself? The USFDA makes its inspection reports publicly available. Why doesn’t India do the same?"
Then, there is also the problem of Indian pharmaceutical companies selling poor-quality products in Africa. In a research report by scientists from the University of Ottawa and the University of Maryland, among others, it was found that Indian manufacturers were likely to sell poor quality in Africa owing to its poor regulations.
“So far, we have discovered two interesting patterns regarding drug quality: First, “made in India" drugs purchased from Africa are of worse quality than those purchased within India, and from non-Africa countries outside of India," writes Roger Bate, Ginger Zhe Jin, Aparna Mathur, and Amir Attaran in their research report titled ‘Poor Quality Drugs and Global Trade: A Pilot Study’. “This pattern is robust to manufacturer-drug fixed effects. Second, the above pattern is mostly driven by non-registered substandard products."
This means India needs to tighten its policies and approval process if it truly wants to emerge as the pharmacy of the world.
“In order to prosecute an erring actor, you first have to fix accountability," say Thakur and Reddy. “This rarely happens in India. More often than not, incidents such as the DEG mass poisoning in Jammu in 2019 are brushed under the carpet just as soon as the attention on the issue subsides. The new amendment which the Ministry of Health proposed in 2022 to the Drugs and Cosmetics Act would make this even worse. It would essentially tie the hands of any well-meaning inspector and take away whatever little ability it has to hold the erring company accountable. One really needs a fundamental relook at the Drugs and Cosmetics Act ground up to address this very serious issue."
Hopefully, the recent fiasco that has dented India’s image globally will be a wake-up call for both companies, and the regulator alike.
First Published: Oct 11, 2022, 15:26
Subscribe Now